Transcranial Magnetic Stimulation: A Noninvasive Approach to Treating Depression
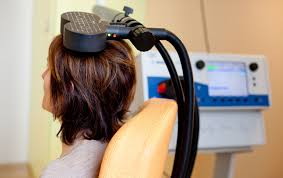
Table of Contents
- Introduction to Transcranial Magnetic Stimulation
- How TMS Works
- Effectiveness of TMS in Treating Depression
- Duration and Frequency of TMS Treatments
- Potential Side Effects and Risks
- Comparing TMS to Other Depression Treatments
- Insurance Coverage and Accessibility
- Conclusion
Introduction to Transcranial Magnetic Stimulation
Depression remains one of the most persistent and challenging mental health conditions worldwide, affecting millions of individuals each year. For many, traditional treatments like medication and psychotherapy provide limited or no relief. In recent years, Transcranial Magnetic Stimulation (TMS) has emerged as a promising noninvasive option for those seeking alternatives. TMS in Colorado has become more accessible as clinics and specialists recognize the demand for innovative mental health therapies.
TMS utilizes magnetic fields to stimulate nerve cells in the brain, specifically targeting regions associated with mood regulation and emotional control. This noninvasive procedure has garnered attention not only for its effectiveness in addressing major depressive disorder (MDD) but also for its minimal side effects and suitability for individuals who haven’t responded to standard therapies. Rather than relying solely on medication or intensive interventions, TMS bridges the gap as a safe, outpatient option with a growing evidence base.
read more : Understanding Dental Emergencies: When to Seek Professional Help
How TMS Works
The science behind TMS is rooted in neurostimulation. During a typical session, an electromagnetic coil is positioned against the patient’s scalp, generally near the forehead. This coil delivers carefully controlled magnetic pulses to stimulate nerve activity in specific brain regions known to have reduced function in depression. While researchers are still clarifying the exact mechanisms, it is believed that these pulsations reinvigorate the neural circuits responsible for mood control, gradually easing depressive symptoms over time.
One of the standout qualities of TMS is its noninvasive nature—unlike more intensive treatments, there is no need for anesthesia or recovery time. Patients remain awake and alert throughout, usually reporting only mild sensations at the treatment site. For individuals wary of pharmaceutical side effects or those unable to tolerate antidepressants, TMS provides a much-welcomed alternative.
Effectiveness of TMS in Treating Depression
Clinical research underscores the efficacy of TMS in treating major depressive disorder. According to data from UCLA Health, around 54% of patients undergoing TMS therapy achieved a notable clinical response—defined as a 50% or greater reduction in depressive symptoms. This level of improvement is particularly striking among individuals considered treatment-resistant, who have struggled with multiple trials of antidepressant medications without satisfactory results.
Compared to traditional treatment pathways, TMS stands out for its rapid onset of action in many patients. Benefits can often be noticed within the first few weeks of therapy, with some experiencing marked relief after only a handful of sessions. This swift response is vital for those in acute distress, as early improvement translates to better overall outcomes and a higher quality of life.
Duration and Frequency of TMS Treatments
A standard TMS protocol typically consists of daily sessions, five times per week, for four to six weeks. Each appointment lasts between 30 and 60 minutes, depending on the specific technology and treatment plan. The cumulative impact of repeated stimulation is crucial to sustaining improvements, with many patients continuing to feel better for months, or even longer, after completing their course.
Follow-up or maintenance sessions may be recommended for some individuals, especially those with a history of recurrent depressive episodes. This tailored approach maximizes long-term wellness while minimizing exposure to medication side effects and the need for lengthy hospital stays.
Potential Side Effects and Risks
TMS is recognized for its favorable safety profile. The majority of users report only temporary side effects, such as mild headaches or scalp discomfort at the stimulation site. These symptoms generally subside after a few sessions or can be managed with over-the-counter pain relievers. There is a minimal risk of more severe reactions, such as seizures, and such occurrences are extremely rare—primarily limited to those with underlying neurological vulnerabilities. Strict screening and patient selection protocols, as highlighted by the Mayo Clinic, help ensure safety.
Some individuals may experience mild twitching or tingling in the facial muscles during the session, but these effects are not harmful and dissipate rapidly. For most individuals, TMS is a well-tolerated and routine experience, even when it is repeated over multiple weeks of therapy.
Comparing TMS to Other Depression Treatments
When compared with other neurostimulation therapies such as electroconvulsive therapy (ECT), TMS offers several key advantages. Most notably, it requires no sedation or anesthesia; patients can drive themselves to and from appointments and resume their daily activities immediately afterward. Memory impairment, a concern associated with ECT, is not an issue with TMS, making it a more attractive option for individuals concerned about cognitive side effects.
While medication and psychotherapy remain first-line choices, TMS fills an important gap for those who have not found relief. However, it is not suitable for everyone; individuals with certain medical implants, metallic fragments, or specific neurological conditions should be carefully evaluated to determine their candidacy.
Insurance Coverage and Accessibility
Insurance accessibility for TMS has improved significantly as more evidence supports its benefits for depression. Most major insurance plans and Medicare now cover TMS for treatment-resistant depression once standard treatments have proven ineffective. Coverage for conditions outside major depressive disorder, or for off-label use, tends to be more restrictive—patients are encouraged to confirm their eligibility with their providers before starting therapy. The increasing number of specialized TMS clinics and trained professionals also means that access is expanding in both urban and rural regions.
As public awareness grows and regulatory support increases, TMS is likely to become a mainstay in the landscape of modern depression care. Patients should seek facilities with robust safety protocols and experienced clinicians for the best outcomes.
Conclusion
For those suffering from persistent depression, Transcranial Magnetic Stimulation offers a beacon of hope, especially when conventional solutions have fallen short. Its noninvasive approach, strong safety profile, and robust effectiveness make TMS an appealing choice for many. With the expansion of insurance coverage and ongoing research, this innovative therapy is poised to play a pivotal role in mental health treatment for years to come.
